Cataract surgery is one of the most common and successful operations performed anywhere in the world. During the procedure, a surgeon removes the eye’s cloudy natural lens and replaces it with a tiny, clear implant called an intra‑ocular lens (IOL). For most people the improvement is almost immediate; colors look brighter, glare is reduced and reading is easier. However, no surgery is completely risk‑free, and a small percentage of people experience problems with their replacement lens months or even years after the operation. These complications can make vision blurry again, create bright streaks or shadows in peripheral vision or even dislocate the lens. While frightening, these issues are usually treatable when recognized early.
This in‑depth guide explores the most common reasons a cataract lens replacement can fail, the symptoms you might notice and the steps you and your eye care team can take to fix the problem. By understanding the risk factors and treatment options, you can advocate for your eye health and maintain clear vision after cataract surgery.
Understanding Cataract Surgery and Intra‑ocular Lenses
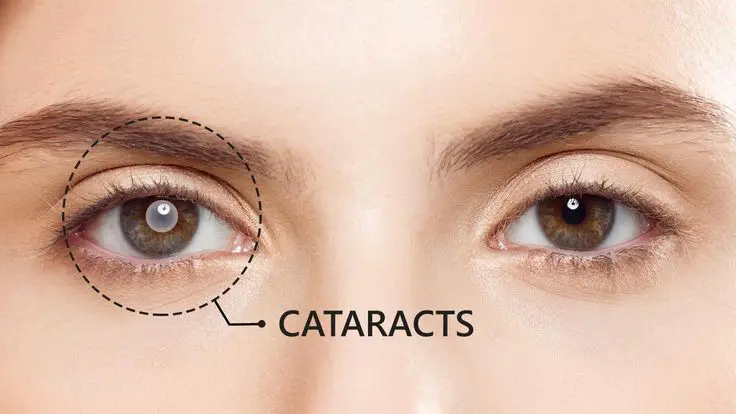
Cataract surgery involves replacing your eye’s cloudy lens with a clear plastic lens. The procedure has become increasingly sophisticated, with improved surgical techniques and biocompatible materials leading to excellent outcomes. According to a large systematic review, millions of cataract surgeries are performed worldwide each year. The artificial lenses used in these surgeries are made from different materials, primarily acrylic or silicone, and are designed to last a lifetime. They come in different designs, including monofocal lenses that correct vision at one distance, toric lenses that correct astigmatism and multifocal or extended depth‑of‑focus lenses that reduce the need for glasses at multiple distances.
How the Lens Is Placed
During the operation the surgeon makes a tiny incision in the cornea and uses ultrasound to break apart the cloudy lens. The pieces are removed, and the new lens is folded and inserted through the same opening. It unfolds inside the lens capsule—the membrane that held your natural lens—where flexible arms called haptics keep it centered. Once inside, the new lens typically stays in place thanks to gentle pressure from surrounding structures.
Expected Recovery
Most patients notice clearer vision within days and full healing within weeks. The American Academy of Ophthalmology notes that risks include infection, bleeding, swelling, retinal detachment and lens dislocation. Doctors instruct patients to use prescription eye drops, avoid strenuous activity and wear a protective shield during sleep. Following these guidelines helps prevent complications.
Despite technological advances, some patients encounter issues that require further treatment. We will examine these complications in detail below.
Common Reasons a Cataract Lens Fails
Several distinct problems can make an intra‑ocular lens stop working as intended. They range from mechanical failures (like the lens moving out of position) to biological changes (such as scarring or cell growth on the lens capsule). Understanding each condition helps you recognize symptoms and seek prompt help.
1. Intra‑ocular Lens Dislocation
What happens: Intra‑ocular lens dislocation occurs when the implant shifts from its intended position in the lens capsule. It may happen early (within days or months) due to surgical complications or late (years later) because the supportive structures weaken. An American Academy of Ophthalmology article explains that the incidence of lens dislocation after cataract surgery ranges from about 0.2 % to 3 %. Early dislocation often results from improper positioning or trauma; late dislocation is commonly associated with gradual deterioration of the fibers (zonules) that hold the capsule in place, pseudoexfoliation syndrome or previous retinal surgery.
Symptoms: People with a dislocated lens typically report blurry or double vision, feeling that something is off inside the eye or seeing the edge of the lens. Some notice glare or halos at night or find that their glasses no longer correct their vision. In severe cases the lens may move into the vitreous cavity (the gel that fills the back of the eye), which can lead to retinal detachment or bleeding.
Risk factors: Trauma (including falls or blows to the head), pseudoexfoliation syndrome (a condition that weakens connective tissue), connective tissue disorders like Marfan syndrome, high myopia (nearsightedness), prior vitreoretinal surgery and inflammation increase the risk of dislocation. Late dislocations often happen years after surgery as the zonules naturally weaken, especially in older adults.
Diagnosis: Eye doctors diagnose dislocation with a detailed slit‑lamp exam and may use ultrasound or anterior segment OCT imaging to determine the position of the lens. Patients may also undergo a dilated retinal exam to look for associated problems like retinal tears or detachment.
Treatment: Management depends on how far the lens has moved and whether it still provides adequate vision. Small decentrations may not require surgery if vision remains acceptable. Otherwise, surgeons can reposition the existing lens by suturing it to the iris or sclera or by inserting a new lens. The American Society of Retina Specialists explains that minor dislocations might only require observation, while more severe cases often need a lens rescue or replacement combined with vitrectomy. The American Academy of Ophthalmology notes that IOL exchange—removing the old lens and implanting a new one—can restore vision but is not risk‑free. After surgery patients may need to use drops and avoid strenuous activity while the eye heals.
2. Posterior Capsular Opacification (Secondary Cataract)
What happens: Posterior capsular opacification (PCO) is sometimes called a “secondary cataract.” It is not a true cataract; instead, leftover lens epithelial cells grow across the back of the lens capsule, forming a cloudy membrane behind the implant. The Cleveland Clinic reports that PCO is the most common complication of cataract surgery, affecting up to 50 % of people within five years. Because it occurs gradually, many patients think their cataract has returned.
Symptoms: PCO causes cloudy or blurry vision, glare around lights, haloes, difficulty reading and trouble seeing in bright sunlight. Symptoms often resemble the original cataract. Some people notice increased sensitivity to light and require more light for reading. The onset is usually months to years after surgery.
Risk factors: Certain medical conditions make PCO more likely, including diabetes, glaucoma, retinitis pigmentosa, high myopia and uveitis. Children and young adults also have a higher risk because their lens epithelial cells are more active. Surgical factors like leaving lens fibers behind or using a rounded‑edge lens design can increase the risk.
Diagnosis: An ophthalmologist can see the cloudy membrane during a slit‑lamp exam. Patients often present complaining that their vision has “gone cloudy again” or that they see glare at night.
Treatment: The standard treatment is a YAG laser capsulotomy. During this quick, painless office procedure the doctor uses a laser to create a small opening in the cloudy capsule. Vision usually improves immediately. The Cleveland Clinic notes that possible complications of the procedure include retinal detachment, increased intra‑ocular pressure and, rarely, lens dislocation. Patients should follow up after the laser to ensure pressure and retina remain healthy.
3. Residual Refractive Error (Incorrect Lens Power)
What happens: Despite careful measurements, the implanted lens may not perfectly match the eye’s refractive needs. The result is a residual refractive error—myopia (nearsightedness), hyperopia (farsightedness) or astigmatism—that leaves patients dependent on glasses or noticing blurred vision at certain distances. The National Institutes of Health notes that these “refractive surprises” are often managed initially with glasses or contact lenses. If non‑surgical correction fails or the error is large, additional procedures may be considered.
Symptoms: Blurry vision at distance or near, difficulty with night driving and dependence on glasses may signal an incorrect lens power. Patients may also experience visual discomfort or headaches.
Risk factors: Pre‑existing corneal astigmatism, previous refractive surgery (LASIK/PRK), extreme axial length (very long or short eyes) and inaccurate biometry measurements increase the risk. Even slight errors in measuring axial length or corneal curvature can lead to significant refractive error.
Treatment: When glasses or contact lenses do not provide adequate vision, several options exist. The NIH review explains that corneal ablative procedures—photorefractive keratectomy (PRK) or laser in situ keratomileusis (LASIK)—can correct residual refractive error. Another option is to implant a secondary “piggyback” lens in front of the existing IOL or to exchange the original lens for one with the correct power. Each approach has pros and cons, and ophthalmologists tailor treatment to the individual.
4. Dysphotopsia (Unwanted Visual Phenomena)
What happens: Dysphotopsias are unwanted light phenomena that occur after lens implantation. The American Academy of Ophthalmology divides them into positive dysphotopsias (bright streaks, arcs or halos) and negative dysphotopsias (dark crescent‑shaped shadows). Positive dysphotopsias result from light reflecting off the lens edge, while negative dysphotopsias may occur when peripheral light bypasses the lens, creating a shadow on the retina.
Symptoms: Patients may describe flashes or streaks of light, arcs in the peripheral vision, rings or haloes around lights, or a dark crescent or arc in one area of vision. These phenomena can be particularly bothersome at night or in bright sunlight.
Prevalence: Dysphotopsias are common. The AAO notes that up to 49 % of patients experience some degree of dysphotopsia in the early postoperative period. Fortunately, many symptoms improve over time through neuroadaptation, often within four to six weeks, though it may take up to a year for some individuals.
Risk factors: Choice of IOL design and material influences the risk. Rounded‑edge lenses reduce positive dysphotopsias but increase PCO risk, whereas square‑edge designs with textured or frosted edges minimize both PCO and dysphotopsias. Silicone lenses have a lower refractive index than acrylic lenses and may produce fewer optical disturbances. Multifocal and extended‑depth‑of‑focus lenses can cause halos or starbursts because of their diffractive optics.
Management: Many patients adapt and no treatment is needed. When symptoms persist and interfere with quality of life, several solutions exist. Doctors may prescribe pupil‑constricting drops, exchange the IOL for a different design, or perform laser procedures to adjust the capsule. A systematic review reported successful treatment of negative dysphotopsia with laser capsulotomy of the nasal anterior capsule, suggesting the capsule edge may be implicated. IOL exchange has also been used when other measures fail.
5. Lens Opacification (Glistenings and Calcification)
What happens: Some artificial lenses develop small fluid‑filled microvacuoles called glistenings or deposits of calcium that cloud the lens. These phenomena can reduce image quality, cause glare and lead to lens exchange. In hydrophobic acrylic lenses, glistenings are microvacuoles that form within the lens material. An AAO editors’ choice article reported that glistenings were found in 86.5 % of eyes implanted with the AcrySof SN60WF blue light‑filtering lens and that grade 2 glistenings were present in 45.9 % of eyes. Despite the high incidence, the study found no clear difference in visual acuity between eyes with more and fewer glistenings. Factors contributing to glistenings include the blue light‑filtering chromophore, storage conditions and environmental factors during surgery.
In hydrophilic acrylic lenses, calcification can cause opacification. A systematic review notes that losing transparency may lead to decreased contrast sensitivity and visual acuity and sometimes requires lens removal. Rapid temperature changes during storage or transport can cause transient lens clouding; moving a lens from freezing conditions into the warm operating room can lead to temporary haze that usually clears within hours. Chronic calcification, however, results from calcium phosphate deposits forming on or within the lens material. The same review states that careful adherence to manufacturer storage guidelines and avoiding extreme temperature shifts help prevent acute opacification.
Symptoms: Most patients with mild glistenings notice little or no effect on visual acuity. In severe cases, glistenings can cause glare, reduced contrast and poor night vision. Calcification creates a milky clouding that can significantly blur vision and reduce contrast sensitivity. Patients may feel like they are looking through a foggy lens, similar to a cataract.
Diagnosis: Ophthalmologists observe glistenings or calcification using a slit‑lamp microscope. They grade the severity based on the number and density of microvacuoles or deposits. The patient’s subjective complaints and objective measurements guide treatment decisions.
Treatment: Glistenings rarely require surgery; education and reassurance are often enough. Some surgeons favor exchanging lenses with significant glistenings for a different material or design if symptoms are bothersome. For calcification that severely impacts vision, lens exchange is the only definitive treatment. Surgeons may replace the opacified lens with one made from a different material, such as hydrophobic acrylic.
6. Infection and Inflammation (Endophthalmitis)
What happens: Endophthalmitis is a serious inflammation of the eye’s internal structures, usually caused by bacterial or fungal infection. While uncommon, it can threaten sight and is considered a medical emergency. The Cleveland Clinic notes that eye surgery, including cataract surgery, is one of the most common causes of exogenous endophthalmitis. Other causes include eye trauma and intra‑vitreal injections. When infection spreads through the bloodstream to the eye it is called endogenous endophthalmitis; this is rare and typically occurs in people with severe systemic infections.
Symptoms: Signs include pain, redness, decreased vision, photophobia, swollen eyelids and discharge. These symptoms usually appear within a week of surgery for acute endophthalmitis or develop slowly for chronic cases. A sudden decline in vision accompanied by severe eye discomfort after cataract surgery warrants immediate evaluation.
Diagnosis: Doctors perform a comprehensive eye exam and may take fluid samples from the aqueous or vitreous humor to identify the infectious organism. Imaging, such as ultrasound, may be used if view of the retina is limited by inflammation.
Treatment: Endophthalmitis is treated urgently with intravitreal antibiotics or antifungals and corticosteroids. Severe cases may require vitrectomy surgery to remove infected material and inject medications into the eye. Early treatment improves outcomes; delays can result in permanent vision loss. Cleveland Clinic experts emphasize that prompt medical care is critical if symptoms occur. After treatment, patients need frequent follow‑up to monitor for recurrent infection or complications.
7. Other Complications and Risk Factors
In addition to the major issues above, several other problems can compromise a replacement lens:
- Iris or pupil problems: Some people develop inflammation that causes the pupil to stick to the lens or iris to the capsule. This can lead to irregular pupil shape, glare or pain. Steroid drops and dilating drops typically control the inflammation.
- Glaucoma and increased eye pressure: YAG laser capsulotomy can sometimes raise intra‑ocular pressure. Patients should have their pressure checked after the procedure. Certain lens designs may also influence aqueous outflow.
- Retinal detachment: Both the AAO and Cleveland Clinic note that retinal detachment is a possible complication of cataract surgery. Dislocated lenses, vitreous loss or high myopia increase the risk. Symptoms include flashes of light, floaters and a curtain or shadow across the field of vision.
- Suprachoroidal hemorrhage: This rare but serious bleeding behind the retina can occur during or after surgery. It may cause sudden pain and vision loss and requires emergency surgery.
- Macular edema: Cystoid macular edema—swelling in the retina’s central area—can occur after surgery or IOL exchange. It causes blurred central vision and may be treated with anti‑inflammatory drops or injections. The IOL exchange study mentioned that two patients developed temporary cystoid macular edema after their exchange.
- Persistent dry eye or ocular surface disease: Pre‑existing dry eye can worsen after surgery and may blur vision. Treatment includes lubricating drops, anti‑inflammatory medications and lid hygiene.
By understanding these potential problems, you can watch for changes in your vision and seek care promptly.
What to Do If You Experience Problems
Discovering that your vision is blurred again or that light phenomena persist after cataract surgery can be distressing. The good news is that most problems have solutions. Here is what to do:
- Contact your ophthalmologist immediately. Any sudden decrease in vision, pain, redness or visual phenomenon should be evaluated promptly. Early diagnosis leads to better outcomes.
- Schedule a comprehensive exam. Your eye doctor will use special microscopes and imaging to assess the lens position, clarity and surrounding structures. Diagnostic tests may include slit‑lamp exam, dilated fundus exam, ultrasound and OCT imaging.
- Follow treatment recommendations. Depending on the cause, treatment may involve observation, laser procedures, medications or surgery. For example, a YAG laser capsulotomy for PCO can restore clear vision, while lens repositioning or exchange can correct dislocation.
- Adhere to postoperative instructions. Use prescribed drops, avoid heavy lifting or straining and wear eye protection when recommended. Infections like endophthalmitis require strict adherence to medication schedules.
- Ask about second opinions. If you are unsure about your options, consider consulting a specialist in cataract and refractive surgery. Complex cases may require the expertise of a retina surgeon, especially when the lens has fallen into the vitreous cavity.
Preventing Lens Replacement Failure
Many complications are unavoidable, but you can reduce your risk by taking proactive steps:
- Choose an experienced surgeon. Surgeons with extensive cataract surgery experience have lower complication rates. Ask about their experience and the types of lenses they use.
- Disclose your medical history. Tell your surgeon about any conditions like pseudoexfoliation, connective tissue disorders, high myopia, uveitis or previous eye surgeries. These factors influence lens choice and surgical technique.
- Follow preoperative and postoperative instructions. Stop medications only under medical advice, use antibiotic and anti‑inflammatory drops as prescribed and avoid rubbing your eye. The AAO recommends avoiding getting water directly in the eye and wearing a shield during sleep.
- Attend follow‑up visits. Regular postoperative checks allow your doctor to detect problems early. PCO, for instance, may develop gradually over months or years. Early laser treatment can restore vision before everyday activities are affected.
- Protect your eyes. Wear protective eyewear when playing sports or doing work that risks eye injury. Trauma is a common cause of lens dislocation. During recovery, avoid heavy lifting or activities that increase eye pressure.
- Maintain overall eye health. Manage systemic conditions like diabetes, which increase the risk of postoperative complications. Eat a balanced diet rich in antioxidants, wear UV‑blocking sunglasses and stay hydrated. A healthy ocular surface promotes better healing and reduces the likelihood of dry‑eye‑related visual issues.
By taking these steps and staying alert to changes in vision, you can help ensure that your cataract surgery outcome remains successful.
When to Consider an IOL Exchange
An intra‑ocular lens exchange involves removing the implanted lens and replacing it with another. This procedure is more complex than the original cataract surgery because the eye has already healed and scar tissue may be present. Surgeons recommend an exchange when other measures—like glasses, contact lenses, laser treatments or lens repositioning—fail to provide satisfactory vision. The Duke Health article notes several reasons for exchange: mechanical failure or dislocation, trauma, capsular tear during the original surgery, pseudoexfoliation syndrome and patient dissatisfaction with visual quality. Premium multifocal lenses are sometimes exchanged for monofocal lenses if patients cannot adapt to halos or other dysphotopsias.
An exchange may also be necessary when the lens becomes opacified due to calcification or when severe residual refractive error cannot be corrected by corneal procedures. Studies show that dislocation is the main overall reason for exchange, while presbyopia‑correcting lenses are often removed because of lens‑induced visual disturbances. Outcomes are generally positive; the same study found that both monofocal and multifocal lens recipients had improved visual acuity after exchange.
Because exchanging a lens carries risks, surgeons carefully evaluate the benefits versus potential complications. Intraoperative challenges include adhesions between the lens and capsule, zonular weakness and risk of vitreous loss. Postoperative complications may include retinal detachment, cystoid macular edema and re‑dislocation. Patients should discuss the procedure thoroughly with their surgeon and consider a specialist center with experience in complex cataract cases.
Living With a Replacement Lens
Most people live happily with their intra‑ocular lens after cataract surgery. If you experience side effects, remember that many are temporary and will improve with time. Neuroadaptation helps your brain adjust to new optical conditions, especially with multifocal or extended depth‑of‑focus lenses. Regular eye examinations remain important; they allow your ophthalmologist to monitor eye pressure, retinal health and lens clarity. If you have chronic conditions like glaucoma or diabetic retinopathy, continued monitoring will ensure these diseases are managed properly.
In cases where visual disturbances persist, specialists can offer solutions. For example:
- For halos or glare: Pupil‑constricting drops, laser procedures to adjust the capsule or lens exchange may help. Some surgeons use a laser to roughen the lens edge, reducing internal reflections.
- For negative dysphotopsia: Laser capsulotomy on the nasal side or adding a reverse optic may reduce the temporal shadow. Lens exchange is considered when other treatments fail.
- For residual refractive error: Laser eye surgery or implanting a secondary lens can sharpen vision when glasses are inadequate.
- For glistenings: Severe cases may benefit from lens exchange to a material less prone to microvacuole formation.
- For PCO: A quick laser capsulotomy restores clarity by removing the hazy membrane.
Partnering with your eye care provider ensures you receive personalized advice and timely treatment.
Conclusion and Actionable Takeaways
Cataract surgery has transformed the lives of millions of people, restoring clarity and color to their world. Yet, as with any operation, complications can occur. Replacement lens failures—whether due to dislocation, posterior capsular opacification, residual refractive error, dysphotopsias, opacification, infection or other issues—can cloud vision and cause frustration. Fortunately, understanding the causes and treatments empowers you to act quickly.
Here are key points to remember:
- Monitor your vision: Pay attention to changes like blur, glare, shadows or pain. Early symptoms often signal treatable problems.
- Attend follow‑up visits: Regular check‑ups allow your doctor to spot and address issues like PCO or high eye pressure before they worsen.
- Report problems promptly: Serious conditions like endophthalmitis require immediate treatment to prevent permanent vision loss.
- Understand your lens: Ask your surgeon about the type of IOL you will receive. Factors like edge design and material influence the risk of dysphotopsias.
- Consider lifestyle and health: Manage systemic diseases, wear protective eyewear and follow all pre‑ and postoperative instructions to minimize complications.
With vigilant care and professional guidance, most people maintain excellent vision after cataract surgery. Should problems arise, modern ophthalmology offers effective solutions—from lasers and medications to advanced surgical techniques. By staying informed and proactive, you can continue enjoying clear, comfortable vision for years to come.

