When Spring Shows Up in Your Eyes

Every April or May, pollen counts rise and millions of people start sneezing and rubbing their eyes. If you’ve ever wondered whether allergies can affect your vision, the short answer is yes. Allergic reactions can set off a cascade of events that irritate your eyes, make them watery or itchy and even blur your vision. In this article we’ll explore why this happens, what eye allergy symptoms look like, and how to find relief. We’ll also discuss when blurry vision is a sign of something more serious and why seeing an eye doctor matters.
What Happens During an Eye Allergy?
When your body encounters an allergen like pollen, dust or pet dander, your immune system treats that harmless substance as a threat. It releases histamines, chemicals designed to help the body fight off invaders. Histamines cause small blood vessels in the eyes to leak and the tissues to swell. That’s why your eyes may become red, watery and itchy. Dr. Marissa Locy from the University of Alabama at Birmingham explains that histamines cause inflammation in the eyes, leading to redness, watering, irritation, itching, light sensitivity and sometimes blurred vision.
Did you know? Allergic conjunctivitis (eye allergy) affects up to 10–30 % of the general population and is one of the most common conditions seen by eye doctors.
Signs and Symptoms: More Than Just Itchy Eyes
Eye allergies aren’t just uncomfortable; they can temporarily affect how clearly you see. Common symptoms include:
- Itching and burning. Itching is the hallmark sign of allergic conjunctivitis. The urge to rub your eyes can be strong, but rubbing worsens swelling and can even scratch the cornea.
- Redness and swelling. Histamine causes tiny blood vessels in the eye’s surface to leak fluid and swell, turning the whites of your eyes pink and making your eyelids puffy.
- Watery or dry eyes. You might think watery eyes indicate too many tears, but watery eyes can actually be a sign of dry eye. Locy notes that the brain sometimes responds to perceived dryness on the cornea by producing excess tears.
- Blurry or fluctuating vision. Swollen eyelids, watery discharge and mucus on the cornea can blur your vision temporarily. Allergic conjunctivitis can also cause sensitivity to light.
- Foreign body sensation. Many people describe feeling like something is stuck in the eye due to swelling and mucus.
Seasonal vs. Perennial Allergic Conjunctivitis
There are several subtypes of eye allergies. Seasonal allergic conjunctivitis (SAC) is the most common. It flares up in spring, summer or fall when pollen counts spike. Symptoms include itching, redness, burning and watery discharge. Perennial allergic conjunctivitis (PAC) occurs year‑round and is triggered by indoor allergens like dust mites, pet dander or mold. The symptoms are similar but often milder.
Other, less common forms include vernal keratoconjunctivitis (VKC) and atopic keratoconjunctivitis (AKC), which are chronic and can threaten vision if untreated. Vernal keratoconjunctivitis often affects boys and young men; symptoms include significant tearing, thick mucus and photophobia. AKC affects older patients with a history of eczema, causing intense itching, burning and thick discharge. Giant papillary conjunctivitis (GPC) is associated with contact lens wear and leads to large bumps on the inner eyelid, causing itching, puffiness and blurred vision.
How Allergies Blur Your Vision

Blurred vision during allergy season usually isn’t caused by damage to the eye, but rather by temporary factors:
- Swelling and tears. When histamine causes the conjunctiva to swell, the smooth optical surface of the eye becomes irregular. Excess tears and mucus can smear across the cornea, scattering light and reducing clarity.
- Dry eye cycle. Allergies and dry eye often occur together. Dr. Tasha Schellenberg at the Dean McGee Eye Institute notes that antihistamines used to treat allergies can decrease tear production, leading to dry eye. In turn, dry eye means the corneal surface is less protected from allergens, causing more inflammation. This cycle of dryness and inflammation can cause blurred or fluctuating vision.
- Contact lenses. Contact lens wearers are prone to GPC, where proteins and allergens accumulate on the lens surface. The resulting bumps on the inner eyelid cause blurred vision and lens discomfort.
Blurred vision from allergies is usually temporary. However, chronic rubbing and inflammation can damage the cornea or contribute to conditions such as keratoconus, which thin the cornea and distort vision. If your blurred vision persists or is accompanied by pain, consult an eye care professional to rule out infection or other eye diseases.
Common Triggers: What Makes Your Eyes React?
Eye allergies can be triggered by a variety of substances:
| Trigger | Examples & Notes |
|---|---|
| Outdoor allergens | Tree, grass and weed pollen are the main causes of seasonal allergic conjunctivitis. Symptoms spike in spring and early summer when pollen counts are high. |
| Indoor allergens | Dust mites, mold spores and pet dander are common culprits of perennial allergic conjunctivitis. Keeping your home clean and controlling humidity can help reduce exposure. |
| Irritants | Smoke, perfume, diesel exhaust and chemical fumes can trigger eye allergies or worsen irritation. Avoiding smoky environments and using fragrance‑free products may help. |
| Contact lens deposits | Proteins or debris on contact lenses can cause giant papillary conjunctivitis. Regular cleaning and replacing lenses as directed are key. |
| Personal products | Some makeup, lotions or skin care products may contain preservatives or fragrances that irritate the eyes. Switch to hypoallergenic brands if you notice irritation. |
Who’s at Risk?
- People with allergies or atopy. Allergic conjunctivitis often occurs alongside allergic rhinitis, asthma or eczema. Family history and atopic predisposition increase your risk.
- Young adults and children. Seasonal and perennial allergies often start in childhood or adolescence. VKC primarily affects boys aged 5–10, while AKC often appears in adults with a history of eczema.
- Contact lens wearers. Wearing soft lenses for long periods can lead to GPC, especially if lenses aren’t cleaned properly or replaced on schedule.
- People exposed to pollution or smoke. Air pollution and tobacco smoke can irritate the ocular surface and worsen allergic reactions.
Eye Allergies vs. Pink Eye: How to Tell the Difference
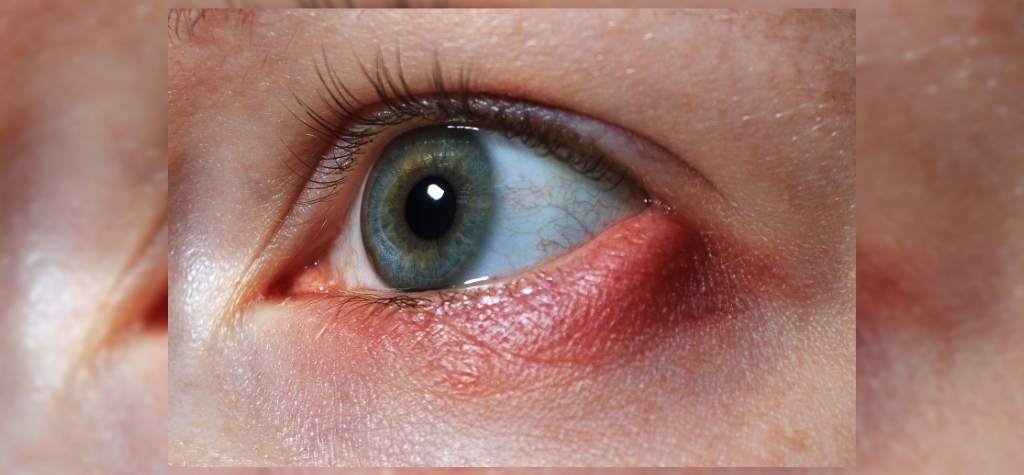
Red, watery eyes can also signal pink eye (conjunctivitis). The National Eye Institute describes pink eye as swelling and redness of the eyelids and the white part of the eye, often accompanied by itching, burning, watery discharge, swollen eyelids, and sensitivity to bright light or blurred vision. Pink eye can be caused by viruses, bacteria or allergies.
Key differences:
- Allergic conjunctivitis usually affects both eyes, causes intense itching and watery discharge, and occurs in conjunction with other allergy symptoms like sneezing. It is not contagious.
- Viral or bacterial conjunctivitis may start in one eye and spread to the other, often produces thicker or yellowish discharge, and can be highly contagious. If you experience pain, pus or severe light sensitivity, see a doctor promptly.
Diagnosing Eye Allergies
Doctors usually diagnose eye allergies based on symptoms and medical history. An allergist may perform a skin or conjunctival scraping test to identify allergy-causing antibodies or white blood cells. Diagnosis is important because eye allergies share symptoms with other eye diseases, and untreated conditions like VKC and AKC can impair vision. If over‑the‑counter remedies don’t help, seeing an eye doctor ensures you receive the right treatment.
Treatment Options: What Works
Treating eye allergies usually involves a multi‑step approach. The American College of Allergy, Asthma & Immunology recommends starting with allergen avoidance when possible:
- Stay indoors when pollen counts are high, especially in mid‑morning and early evening.
- Close windows and use air conditioning to keep pollen and mold out. Clean A/C filters regularly.
- Wear sunglasses outdoors to keep pollen out of your eyes.
- Don’t rub your eyes; it worsens itching and may introduce bacteria.
- Reduce indoor allergens. Use mite‑proof covers on bedding, wash linens in hot water, control indoor humidity to prevent mold and keep pets out of the bedroom.
Home Remedies
For mild symptoms:
- Artificial tears rinse allergens off the eye surface and add moisture.
- Cold compresses reduce swelling and soothe irritation.
- Warm compresses may help if dry eye rather than allergy is the main problem.
- Hydration and diet. Drinking water and eating omega‑3–rich foods (like fatty fish) support tear production.
Over‑the‑Counter (OTC) Medicines
- Antihistamine eye drops quickly relieve itching and redness by blocking histamine; some also contain mast cell stabilizers for longer relief. Examples include ketotifen and olopatadine.
- Mast cell stabilizers (e.g., cromolyn sodium) prevent histamine release; they take longer to work and are better for prevention.
- Combination drops (antihistamine + mast cell stabilizer) provide both quick and long‑term relief.
- Decongestant eye drops reduce redness by constricting blood vessels, but they shouldn’t be used for more than a few days to avoid rebound redness.
- Oral antihistamines may help allergy symptoms but can dry out the eyes and sometimes make symptoms worse.
- Artificial tears with no preservatives help counteract dryness caused by antihistamines.
Expert tip: Over‑the‑counter medicines may not control severe eye allergies. If symptoms persist or vision is impaired, prescription drops or allergy shots may be necessary.
Prescription Treatments
If OTC solutions aren’t enough, doctors may prescribe:
- Stronger antihistamine or mast cell stabilizing drops. These are similar to OTC options but often more potent.
- Non‑steroidal anti‑inflammatory drugs (NSAIDs). Drops like ketorolac reduce inflammation when combined with antihistamines.
- Topical corticosteroids. Short courses of steroid drops relieve severe inflammation but must be used under medical supervision to avoid side effects like increased eye pressure.
- Immunotherapy (allergy shots). For persistent allergies, allergists may recommend shots to desensitize the immune system to specific allergens.
Managing Contact Lens–Related Allergies
For contact lens wearers experiencing GPC, doctors may advise switching to daily disposable lenses, cleaning lenses with fresh solution, or temporarily discontinuing lens wear. A bandage contact lens may also be used to protect the cornea while it heals.
Preventive Habits to Protect Your Vision

- Monitor pollen counts. Check local forecasts and stay indoors during peak pollen periods (usually midday and windy days).
- Use HEPA filters. High‑efficiency air purifiers remove airborne allergens like pollen and pet dander.
- Shower and change clothes after outdoor activities. Pollen sticks to hair and clothing; washing it off reduces exposure.
- Clean bedding and vacuum regularly. Use a vacuum with a HEPA filter to capture dust mites and pet dander.
- Limit contact lens wear during allergy season. Consider glasses if lenses exacerbate symptoms.
- See an eye doctor yearly. Routine check‑ups help diagnose underlying conditions early and ensure your prescriptions are up to date.
When to Seek Medical Help
Most allergy‑related eye symptoms are uncomfortable but temporary. However, contact a health professional if you experience:
- Severe pain, photophobia or thick discharge. These signs may indicate an infection or more serious eye problem.
- Persistent blurred vision. Blurriness that doesn’t improve with blinking or lubricating drops could signal corneal involvement or keratoconus.
- Symptoms lasting longer than a few weeks. Chronic inflammation can damage the cornea and lead to scarring.
- Vision changes with contact lenses. Discontinue lens wear and see your optometrist if you suspect giant papillary conjunctivitis.
Conclusion: Yes—Allergies Can Affect Your Vision
Seasonal and year‑round allergies do more than make you sneeze; they can inflame and irritate your eyes, leading to redness, itchiness, watering and even blurry vision. Understanding the underlying mechanism—histamine release and immune response—helps explain why your vision fluctuates during allergy season. By recognizing triggers, practicing avoidance strategies, using appropriate eye drops and seeking professional help when necessary, you can keep your eyes comfortable and your vision clear. If you experience persistent or severe symptoms, an eye doctor or allergist can provide targeted treatment and help you see the world clearly again.

